A user's guide to heartburn treatment
4/19/2021 by Regina Haeflinger, C.S.T., and Laurel Lake, Pharm.D., R.Ph.
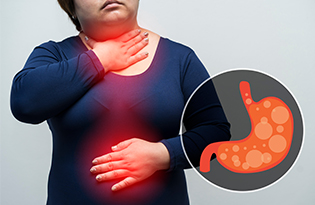
Heartburn is a burning pain often felt behind the breastbone in the middle of your chest. It occurs when stomach acid escapes into the esophagus, which is the tube that brings the food you eat to your stomach.
Where the esophagus meets the stomach is a rubber band like muscle that relaxes when you eat and then tightens again to keep the food and acid in the stomach. In some people, this muscle relaxes too much when a large meal is eaten, or when they lay down on a bed or couch. As a result, this muscle opens, allowing food or stomach acid to enter the esophagus and causing heartburn.
How is heartburn treated?
Nonmedication and medication treatments are available:
- Nonmedication treatment options
The first options used to correct heartburn are simple lifestyle changes, including:- Raising the head of your bed 4-6 inches.
- Wearing loose-fitting clothing.
- Eating smaller meals or eating meals two to three hours before laying down.
- Cutting back on alcohol and smoking.
- Avoiding trigger foods, such as caffeine, tomatoes, chocolate and onions.
- Losing weight.
- Medication treatment options
Three classes of over-the-counter medications are used to treat heartburn:- Antacids, such as Tums or Maalox
- Histamine, or H2, blockers, such as Pepcid or Tagamet.
- Proton pump inhibitors, such as Protonix or Nexium.
For as-needed symptoms, patients may find relief with antacids or histamine blockers. These medications are generally safe and well-tolerated when used as directed or under the direction of your health care provider. Proton pump inhibitors are more powerful medications that are used daily, and they can be used for more frequent symptoms or if other medications do not provide relief.
Should you tell your health care provider about these over-the-counter medications?
You should notify your care team if you take any of these medications. Although many of these heartburn medications are available over the counter, they may interact with other medications you take. Some side effects are associated with long-term use of proton pump inhibitors, and your health care provider may need to perform additional monitoring.
Talk to your health care provider before taking both a proton pump inhibitor and histamine blocker together. If symptoms are severe enough to take multiple medications, you should see your health care provider to make sure it is simple heartburn and not a more severe issue. Taking both medications can increase the risk of gastrointestinal infection and decrease absorption of vitamins and calcium.
Is it time to stop your heartburn medication?
You may need to stay on your proton pump inhibitor long term if:
- You have a history of ulcers, and frequently take medications like aspirin or ibuprofen — both nonsteroidal anti-inflammatory drugs.
- You have Barrett's esophagus (damage to the lower portion of the tube that connects the mouth and stomach).
If you have ben using one of these medications for many months or years for simple heartburn symptoms, it may be appropriate to discuss stopping the medication with your provider.
How can you discontinue these medications?
Medications such as Pepcid or Tums are only to be used as needed, and they can be stopped at any time. When someone has been taking a proton pump inhibitor for longer than three months, it is advised to slowly decrease the dose of the medication instead of quitting cold turkey.
The proton pump inhibitors have been shutting off your acid production, and quitting cold turkey would turn them all on at once, potentially causing an overproduction of acid. Slowly decreasing your daily amount by 50% every 1-2 weeks has been shown to be the best way to successfully taper off these medications.
Regina Haeflinger is a pharmacy student completing clinical rotations at Mayo Clinic. She will graduate from Creighton University in May. She enjoys educating patients and helping them understand their medications.
Laurel Lake, Pharm.D., is a pharmacist completing her residency training in ambulatory care at Mayo Clinic in Rochester.
